Sushant Sadotra
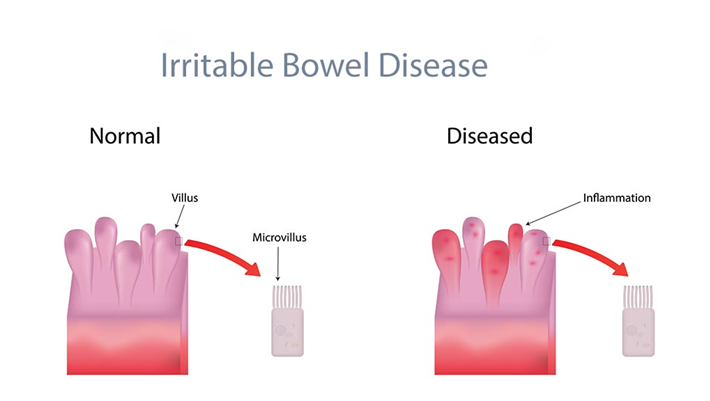
Feline inflammatory bowel disease (IBD) is a chronic condition that affects a cat’s gastrointestinal (GI) tract. The walls of the GI tract become thickened due to the infiltration of inflammatory cells, disrupting the cat’s ability to digest and absorb food properly. Although IBD can affect cats of any age, middle-aged and older cats are more prone to it. The exact cause of IBD remains unknown, but current evidence suggests that it may result from an abnormal interaction between the immune system, diet, bacterial populations in the intestines, and other environmental factors. Genetic abnormalities in the immune system are also believed to play a role in feline IBD, based on similarities to IBD in humans and dogs.
Depending on the region of the GI tract and the type of inflammatory cells involved, IBD can manifest in different forms. If the stomach is inflamed, it is called gastritis; if the small intestine is inflamed, it is called enteritis, and if the colon is inflamed, it is called colitis. Lymphocytic plasmacytic enteritis is the most common form of IBD, where inflammatory lymphocytes and plasma cells attack the small intestine. Eosinophils, another type of inflammatory white blood cell, may also be involved in feline IBD, but are usually part of a mixed population of inflammatory cells. Neutrophilic IBD, which involves neutrophils, and granulomatous IBD, which involves macrophages, are two less common forms of IBD.
In some cases, IBD can cause inflammation of other abdominal organs, such as the liver and pancreas. It is important to identify the type of IBD affecting a cat through appropriate diagnostic procedures to provide the best possible treatment and management.
Clinical symptoms:
Feline IBD is often characterized by a set of common clinical signs that include weight loss, vomiting, decreased appetite, diarrhea, lethargy, and bloody stools. The severity and frequency of these signs can vary depending on which parts of the gastrointestinal tract are inflamed. For instance, if the inflammation is situated in the stomach or higher regions of the small intestine, the cat may experience chronic vomiting. Conversely, inflammation in the colon is more likely to cause diarrhea, with or without blood in the stool.
Diagnosis
When it comes to making a diagnosis of feline IBD, it is important to conduct a thorough workup since many of the symptoms of IBD can overlap with other diseases. To determine the root cause of the symptoms, your veterinarian will most likely recommend conducting baseline blood work, fecal examinations, X-rays, or an abdominal ultrasound to check for metabolic disease, feline leukemia, parasitic or bacterial infections, hyperthyroidism, and certain types of cancer.
Intestinal lymphoma, a form of cancer, can be particularly challenging to distinguish from IBD in cats. Additionally, a veterinarian may also measure the levels of B vitamins B12 and folate in the bloodstream, as IBD can hinder the absorption of these vitamins from the GI tract. Finally, a hypoallergenic food trial may be conducted to rule out food allergy as a possible cause.
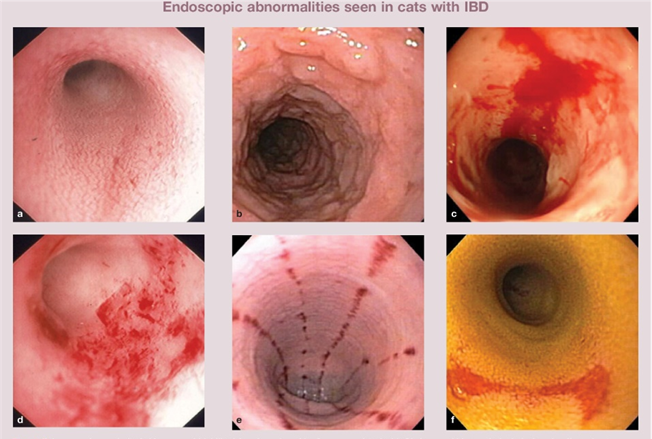
To further diagnose feline IBD, a biopsy is required to evaluate the tissue under a microscope. Increased numbers of inflammatory cells in the intestinal wall indicate the presence of IBD. Endoscopy and surgery are two methods of performing gastrointestinal biopsies, both of which require general anesthesia. However, surgery may be recommended for patients with suspected liver or pancreatic disease to biopsy these organs as well.
Treatment
If you suspect that your furry friend has intestinal parasites, it is important to consult with a veterinarian who will recommend appropriate treatment. The initial steps usually involve a combination of dietary changes and medications. Since there is no one-size-fits-all solution, your vet may need to experiment with different diet and medication combinations to determine the best therapy for your pet.
Dietary Management
If your cat is suffering from Inflammatory Bowel Disease (IBD), it is likely that dietary allergens are playing a role. Your veterinarian may suggest undergoing a food trial using hypoallergenic diets to help alleviate the symptoms. These diets include protein or carbohydrate sources that your cat has never consumed before. Some common initial choices are diets based on rabbit, duck, or venison. In case the symptoms do not improve with a hypoallergenic diet, your cat may benefit from diets that are high in fiber, low in fat, and easily digestible. It is important to note that it may take several weeks or even longer for your cat to show signs of improvement after a diet change. During any food trial, it is crucial to eliminate all other food sources, including table scraps, flavored medications, and treats.
Medical Treatment
- Inflammatory bowel disease (IBD) is a common ailment among cats that can cause chronic gastrointestinal (GI) issues. To treat this condition, veterinarians often recommend a combination of dietary modification and medication.
- Metronidazole is usually the first medical therapy recommended along with dietary modification. This drug has antibiotic, anti-inflammatory, and antiprotozoal properties and is generally well-tolerated by cats. However, some cats may lose their appetite when given this medication. If dietary modification or metronidazole are not effective, corticosteroids may be recommended.
- Corticosteroids are potent anti-inflammatory and immune-suppressing agents that can be administered alone or in combination with metronidazole. However, cats who take these drugs should be closely monitored due to potential side effects such as diabetes and immune suppression. Cats typically take corticosteroids orally, starting with a high dose that is gradually reduced over several weeks. If a cat won’t take medication orally or suffers from severe vomiting, the veterinarian may give the medication as an injection.
- If neither metronidazole nor corticosteroids are effective in controlling the symptoms of IBD, more potent immunosuppressive drugs such as chlorambucil or azathioprine may be necessary. However, these drugs can suppress the production of blood cells, and a veterinarian must carefully monitor cats taking these medications.
- To promote GI health, newer therapies include prebiotics, which promote certain bacterial populations, and probiotics, which are bacterial strains that promote GI health. The addition of soluble fiber, such as psyllium, to the diets of cats with inflammatory colitis may also be helpful. Additionally, cats with IBD should be supplemented with folate or vitamin B12 if they are deficient in these B vitamins.
- Overall, it’s important to work closely with a veterinarian to determine the best course of treatment for your cat’s IBD symptoms.
Reference
- https://www.vet.cornell.edu/departments-centers-and-institutes/cornell-feline-health-center/health-information/feline-health-topics/inflammatory-bowel-disease#:~:text=Feline%20inflammatory%20bowel%20disease%20(IBD,properly%20digest%20and%20absorb%20food.
- https://www.brookfieldanimalhospital.com/project/inflammatory-bowel-disease-in-cats/
- https://www.semanticscholar.org/paper/Feline-Idiopathic-Inflammatory-Bowel-Disease-Jergens/08d34b7a12ac2f59afe5ec3bca4940afea9c6a58/figure/2

